Is Uganda on track to win the COVID-19 battle or is the worst yet to come?
5 May 2020

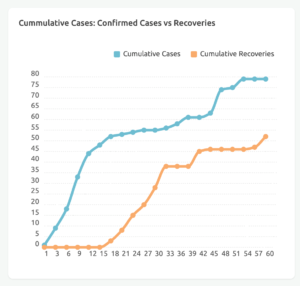
Uganda has so far reported 79 cases of COVID-19 since the first case was reported on 21 March 2020. Notably, among the cases there are no health workers, no deaths and 52 of them have recovered and returned to their homes (66% recovery rate). The first wave of suspected cases were travelers who returned through Entebbe International airport (Uganda’s only airport). Disease transmission amongst this group was successfully interrupted through their institutional quarantine or self-isolation, testing and hospitalization of those found to be positive, coupled with tracing and testing of their contacts and subsequent quarantine or hospitalization for those who tested positive for COVID-19. This was further enhanced through nationwide lockdown.
A whole-of-government approach is being used to address the COVID-19 pandemic, building on past experiences of responding to Ebola and Marburg outbreaks. The response is being championed by a multisectoral national task force coordinated by the Honourable Prime Minister. Decisions are guided by science championed by Ugandan scientists in government ministries and agencies, universities and research institutions, with support from the World Health Organization, other development partners and non-governmental organisations. The president of Uganda was quick to announce a lockdown to curtail transmission among the first wave of cases, and to allow the national task force to get a better understanding of the disease transmission dynamics as well as prepare the health system to handle COVID-19 cases while continuing to provide essential health care services. Consequently, interruption of transmission from the first wave of cases to the community appears to have been successful.
However, the country is now grappling with a new wave of cases of commercial truck drivers from neighbouring countries who have been found to have COVID-19 upon being tested by Uganda health authorities at various border crossing points. Another potential risk group are refugees that traverse the country borders. Despite the government ban on movement to and from refugee settlements, one of the confirmed cases is a refugee resident in Uganda who was detected on his return from Tanzania. The cross-border movements that are happening amidst soaring COVID-19 cases in neighboring Tanzania and Kenya threaten to undo Uganda’s gains. This calls for an East African Regional approach to the fight against COVID-19 pandemic. Could these trans-border cases be the beginning of the surge that was predicted?
In the event that Uganda actually experiences a surge of COVID-19 cases as has been predicted for African nations, the country is racing against time to address critical logistical, infrastructural and human resource challenges in its health system. These include inadequate stocks of Personal Protective Equipment (PPEs), the need to train all health workers on COVID-19 response, an acute shortage of critical care nurses, a lack of intensive care unit (ICU) beds and a lack of reliable and consistent oxygen supplies in health facilities. Some of the regional referral hospitals that are designated to manage COVID-19 cases lack ICU beds. As of early 2020, there were only 55 functional ICU beds in Uganda which translates to 1.3 ICU beds per million population. [1]
THET’s Health Worker Action Fund launched last month provides a timely and viable option for addressing these health systems gaps through Health Partnerships between UK and Ugandan institutions.
Uganda’s leadership and frontline workforce have demonstrated a resolve to combat COVID-19 despite the prevailing health system challenges.


1 Comment
Leave a comment
Your email address will not be published.